Vita Sara Plechner’s life changed one Saturday afternoon. A middle school librarian, she was at home in Oceanside, New York, when she experienced a sharp pain in her back. An antacid didn’t ease the burning sensation, so she went to the emergency room.
That was March 7, 2020, just days before New York City hospitals became like war zones due to the coronavirus pandemic. Doctors performed an ultrasound and a CT scan on Plechner, then 67 years old. The results showed she had a tumor in her pancreas. She was devastated because she didn’t drink, didn’t smoke, and led a healthy lifestyle.
After two days in the hospital, she returned home and began to consider her limited options. Pancreatic cancer is among the deadliest forms of cancer; only one in four patients survives for a year after diagnosis, and only one in ten survives for two years.
Blechner felt the weight of these numbers and sat down with her husband and three adult children to make calls and do online research to determine her next step. Ultimately, she chose a rapidly evolving, yet often misunderstood, path in cancer research.
Messenger RNA (mRNA) is a single-stranded molecule that carries genetic information from DNA to direct protein synthesis. Most people are familiar with it from school science lessons or its use in COVID-19 vaccines.
But long before COVID-19, this field was generating considerable excitement among cancer researchers. BioNTech, the German company that designed the COVID-19 vaccine for Pfizer, developed it using a platform it had been using to develop cancer treatments for about a decade.
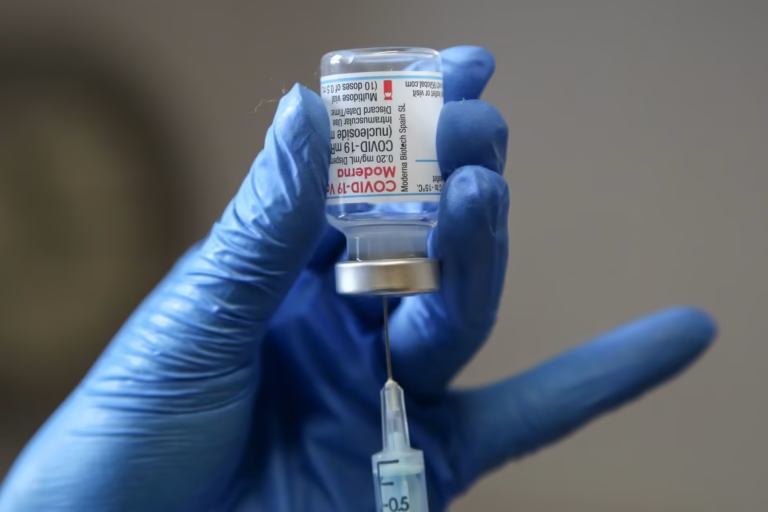
While the mRNA-based COVID-19 vaccines developed by Pfizer and Moderna mitigated the pandemic’s impact, they also triggered political backlash over the past year, threatening to slow down or derail dozens of potential cancer treatments. But after a turbulent 12 months, there are signs that this trajectory is continuing.
“It’s exciting,” said Elizabeth Jaffe, deputy director of the Sidney Kimmel Comprehensive Cancer Center at Johns Hopkins University. “We’ve seen a number of successes in early trials and positive results.”
Katherine Wu, a professor at the Dana-Farber Cancer Institute and Harvard Medical School, noted that the recent positive results contributed to the National Cancer Institute’s announcement of $200 million in funding for the development of new cancer vaccines.
“We’re receiving tremendous support from the National Cancer Institute for the development and advancement of cancer vaccines, and mRNA vaccines are a key part of that effort,” Wu added.
A cruel enemy
To determine her treatment plan, Plechner turned to doctors at Memorial Sloan Kettering Cancer Center, including Vinod Balachandran, director of the Olayan Center for Cancer Vaccines, who said that developing a vaccine against cancer is more complex than developing a vaccine against a virus or bacteria, because it is connected to the immune system, which is primed to recognize viruses and pathogens as foreign bodies. Therefore, the vaccine trains the body to do something it is already prepared for. Cancer, however, is part of the body itself, originating from our own tissues. Most of Balachandran’s research over the past two decades has focused on pancreatic cancers, given the difficulty of this disease. “It’s a type of cancer that treatments haven’t really worked for,” he says.
When Plechner arrived at Memorial Sloan Kettering Cancer Center, Balachandran had already begun a trial of an experimental messenger RNA (mRNA) vaccine for pancreatic cancer, alongside immunotherapy and chemotherapy. He believed that the vaccine’s success could open the door to broader applications, adding, “If we can break through the toughest of them, it could help us understand how to treat other types, because it would provide a model to build upon.”
To develop this vaccine, he began by studying what are known as “exceptional survivors”—less than 10% of pancreatic cancer patients who live more than five years after diagnosis. Their immune systems were found to be more adept at automatically recognizing cancer cells as foreign.
Balachandran explained that these patients have about 12 times more T cells inside their tumors than normal. Unlike other cells, these are a specialized type of immune cell, and in some cases, these cells can remain in the body for more than a decade.
He also discovered that these cells don’t work in a general way, but rather target specific mutations. He says, “These T cells recognized mutations, but each person’s immune system recognizes cancer in a very specific way. To replicate this, we need to teach each individual’s immune system how to recognize their specific cancer. In other words, we need a vaccine tailored to each patient, and we found that the best technology to achieve this quickly was using messenger RNA.”
Participating in a Research Trial
After Plechner agreed to participate in the trial, the first step was a surgical procedure known as the Whipple procedure to remove the tumor from the head of the pancreas. In a laboratory at the center, the tumor was preserved and cut into extremely fine pieces, thinner than a human hair. In less than 72 hours, the sample was sent to Germany, where specialists at BioNTech processed it into a clear liquid—a personalized vaccine specifically designed for Plechner.